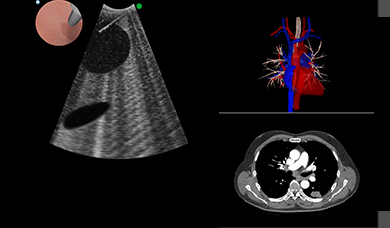
Optimizing Bronchoscopy Training
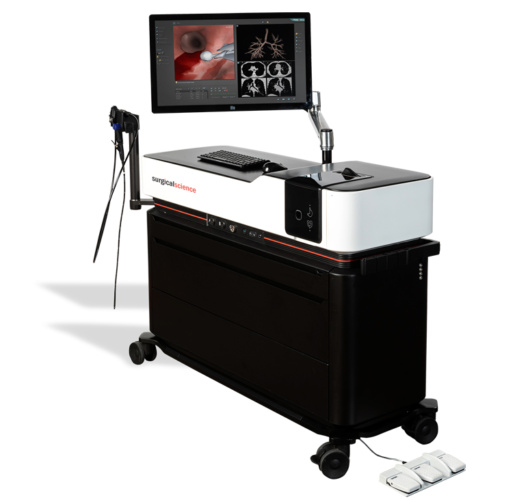
With the BRONCH Mentor simulator you can enjoy a flexible, all-inclusive, and highly reactive training environment.
It provides a comprehensive solution for flexible bronchoscopy training of pulmonary and critical care physicians, thoracic surgeons, anesthesiologists, interventional pulmonologists and others. Fundamental skill tasks and complete clinical procedures provide an optimal learning environment for motor, cognitive and coordinative skills acquisition, as well as diagnostic and therapeutic clinical hands-on experience towards competency.
Diverse Uses for the BRONCH Mentor
Dr. Carla Lamb, Program Director of Interventional Pulmonology Medicine Fellowship and Bronchoscopy at Beth Israel Lahey Health and VP of AABIP talks in this video about the multiple uses for the Simbionix BRONCH Mentor at her center.
Features and Benefits
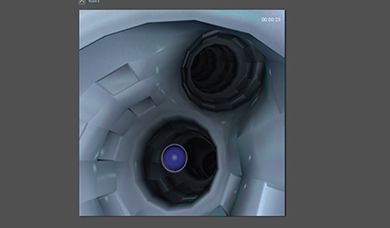
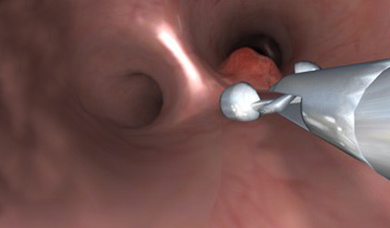
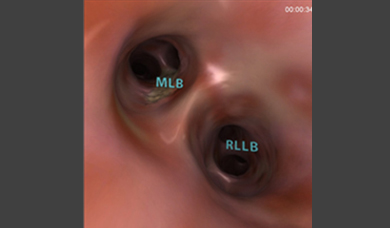
- Realistic and comprehensive bronchoscopic simulation training away from patient, designed to support both team and solo training sessions
- Complete patient management with moderate sedation dynamic complications, and reactive virtual patients
- Didactic environment enhancing the learning curve, including skill-targeted tasks, procedural tasks, aided/un-aded clinical cases – each followed by comprehensive performance feedback
- Includes Essential Bronchoscopy skill tasks module co-developed with AABIP
- Includes CHEST standardized curriculum for essential bronchoscopy skills and diagnostic bronchoscopy, a highly structured training module, co-developed with American College of Chest Physicians
Testimonials
I had the opportunity to train on the BRONCH Express simulator and proctor our first year fellows. The system is extremely easy to use and well designed. The step-by-step learning approach of the simulator…
Prof. Levent Dalar
Site Director, First Interventional Pulmonology Institute, World Association of Bronchoscopy and Interventional Pulmonology (IP-WABIP), Liv Hospital, Istanbul, Turkey
“We are pleased to partner with Surgical Science to deliver a standardized interventional pulmonology curriculum, allowing individual programs to offer training that’s been validated through CHEST’s…
Nicole Augustyne
Senior Vice President of Education of CHEST
“At Loyola University of Chicago Stritch School of Medicine’s Advanced Procedure Education Lab we have a state-of-the-art Surgical Science GI –BRONCH Mentor trainer. It’s an invaluable tool for resident…
Anthony Dwyer
Clinical Skills, Loyola University, Stritch School of Medicine, Chicago, IL.
“Using the BRONCH Mentor and the BRONCH Express in our facility has enabled our trainees to rapidly acquire and adopt safe and efficient bronchoscopy habits. The use of the simulation software facilitates…
George Eapen, MD, FACP, FCCP
Professor of Medicine Section Chief, Interventional Pulmonology Program Director, Department of Pulmonary Medicine. MD Anderson Cancer Center Houston, TX
Validations
The endobronchial ultrasound assessment tool could be used to provide reliable and valid assessment of competence in EBUS-TBNA, and act as an aid in certification. Virtual-reality simulator training was shown to be more effective than traditional apprenticeship training.
The simulator demonstrated validity in differentiating skill in scope manipulation and airway anatomy, but did not discriminate skill levels in anatomic orientation or identification of lymph nodes. Bronchoscopy simulation was viewed as helpful by all levels and should be considered before performance on patients.
Learn More
Download the BRONCH Mentor Brochure
Learn more about the BRONCH Mentor simulator..
Contact Us
Do you want to know more about the BRONCH Mentor?